 Longstanding and poorly managed diabetes can result in the diabetic retinopathy, which refers to the damaged retina, the light sensitive part of eye associated with the formation of vision which presents as vision abnormalities and in untreated cases may culminate in blindness. Proliferative diabetic retinopathy (PDR) is the more advanced phase of diabetic retinopathy. Read on to know the symptoms and preventions of this disease.
Longstanding and poorly managed diabetes can result in the diabetic retinopathy, which refers to the damaged retina, the light sensitive part of eye associated with the formation of vision which presents as vision abnormalities and in untreated cases may culminate in blindness. Proliferative diabetic retinopathy (PDR) is the more advanced phase of diabetic retinopathy. Read on to know the symptoms and preventions of this disease.
Symptoms of Proliferative Diabetic Retinopathy
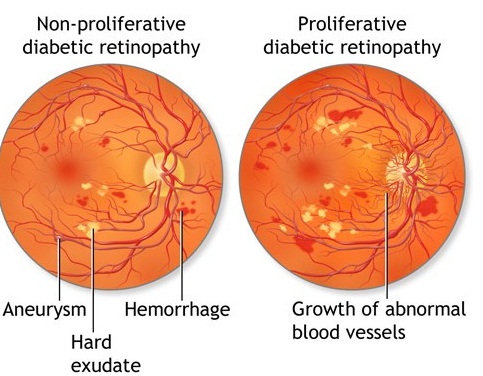
Non – proliferative diabetic retinopathy (NPDR) marks the weakening or retinal blood vessels but no new blood vessel formation takes place during this stage. Proliferative diabetic retinopathy (PDR) is the more advanced phase of retinopathy marked by development of new blood vessels that are leaky, irregular and may increase the risk of complications. In a number of cases, the symptoms of diabetic retinopathy remains concealed until the disease is in advanced stages. Following symptoms points to the development of proliferative diabetic retinopathy:
- Blurring of vision
- Appearance of dark strings or spots in the eyes (floaters)
- Transient or complete loss of vision
- Changes in the quality of color perception
- Development of signs of retinal detachment (sudden episode of extreme pain in the eye followed by blindness)
- Development of cataract
- Appearance of fatty deposits in the retinal vessels (as observed on eye examination)
Complications
Diabetic retinopathy may lead to a variety of complications like:
- New blood vessels that are developed in advanced diabetes may lead to hemorrhage (small hemorrhages are often missed).
- If left untreated, large hemorrhages may lead to retinal detachment due to vitreous hemorrhage
- Development of glaucoma due to new blood vessel formation that leads to headaches, sensation of pressure in the eyes and damage to optic nerve.
- In untreated cases, complete blindness may ensue due to long standing glaucoma or hemorrhage
In order to learn more about proliferative diabetic retinopathy, please refer to this video below:
Causes of Proliferative Diabetic Retinopathy
The primary pathology that leads to vision abnormalities is vascular damage to vessel walls due to high blood sugar levels. The pathological process affects the small vessels first, but then eventually involves large blood vessels; thereby blocking the entire blood supply of retina. This pathological process initiates vision loss that progresses with the formation of new blood vessels within the retina. Since, newly formed blood vessels are leaky and vulnerable to pressure and injuries.
Risk Factors
Following risk factor are most commonly associated with proliferative diabetic retinopathy:
- The risk of diabetic complications increase with advancing age or with prolonged duration of diabetes
- Certain races like African Americans and Hispanics are at higher risk of developing diabetic retinopathy than other races.
- Poorly controlled diabetes (due to non- compliance of drugs or diet) can also lead to diabetic retinopathy.
- If high blood sugar levels are associated with other pathological systemic disorders like hypertension, hypercholesterolemia or physiological condition like pregnancy, the risk of retinopathy and blindness increases many folds.
Preventions for Proliferative Diabetic Retinopathy
The management of proliferative diabetic retinopathy is dependent on the management of diabetes. Following measures should be adopted to manage or prevent proliferative diabetic retinopathy.
Periodic Eye Examination
See a diabetic specialist at periodic intervals to ascertain if the hypoglycemic medications are effective and fully functional. Moreover, see an eye specialist at least once in every 3 months to detect early changes in the visual field.
Quitting Tobacco
It has been observed that smokers are at elevated risk of developing atherosclerosis in the presence of abnormal or poorly managed blood sugar levels. Diabetics are suggested to quit smoking and other hazardous habits like illicit drug abuse and alcohol consumption for optimal blood sugar control.
Blood Sugar Control
Maintain healthy lifestyle by consuming a healthy diet and regular physical activity. Seek the help of a medical or diabetic specialist to know what hypo-glycemic medications are best for you.
Blood Pressure and Cholesterol Control
Diabetics who are also hypertensive or have abnormal lipid metabolism are more vulnerable to develop vascular changes at an elevated rate. It is therefore recommended to manage the serum lipid levels and blood pressure under tight range with the help of medications and lifestyle modification.
Attention to Vision Changes
Vision changes are reported long before the development of full blown diabetic retinopathy. It is recommended to pay extra caution to changes in your vision (like blurring, excessive watering, periodic headaches and appearance of spots in your visual field).
Alternative Medicines for Proliferative Diabetic Retinopathy
So far there has been no proven remedy or therapy that can correct or manage diabetes or diabetic retinopathy. There are some herbal supplements that are helpful in delaying the onset of complications due to long standing diabetes, including
- Gingko biloba
- Grape seed extract
- Bilberry
- Pycnogenol (Pine bark)
- Butcher's broom
For best results, it is recommended to speak to your doctor prior to starting herbal supplements as these agents may interact with your hypoglycemic drugs.
Medical Treatments for Proliferative Diabetic Retinopathy
- Photocoagulation. This procedure involves laser ablation of your retinal neovascularization (new blood vessels in retina) that prevent leaking and hemorrhage.
- Panretinal Photocoagulation. This procedure deals with laser ablation of retinal vessels at sensitive spots like retina. Laser burns shrink and coagulate new vessels that delay the onset of full blown complications.
- Vitrectomy. Vitrectomy involves introducing an incision along your vitreous cavity to remove accumulated blood and scar tissue that is produced as a result of hemorrhage. It can also be used to remove gas bubble or other debris that may lead to retinal detachment in untreated cases.
- Ovine Hyaluronidase Therapy. In case of moderate vitreous hemorrhage, the injection of Ovine Hyaluronidase is helpful in managing the symptoms in 70% of the subjects.
- Bevacizumab Therapy. Bevacizumab is known to manage the symptoms of neovascularization, vitreous hemorrhage and optic nerve damage.
